Acne can be frustrating, especially when it does not go away after your teenage years. Believe it or not, acne can continue to affect adults beyond adolescence, or develop for the very first time in adulthood. This may be particularly distressing for adult women, who are more likely to get acne after the age of 20 compared to men.
What is adult female acne?
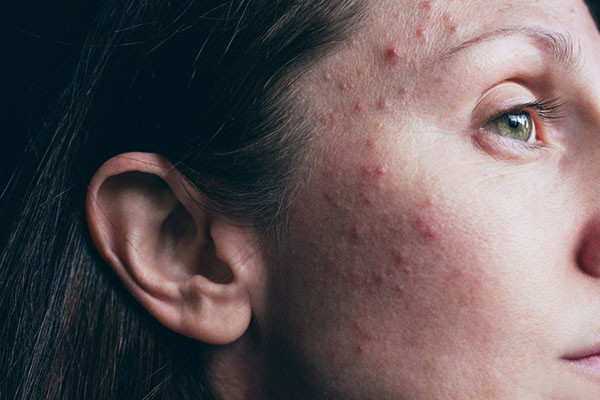
Adult female acne can look very similar to teenage acne. While adult acne is commonly thought to affect the jawline and chin, it can appear on any part of the face or trunk. Adult women can have clogged pores, inflamed pus-filled bumps, or deep-seated cysts. Unfortunately, treatment options that worked well in the teenage years may not work as well in adult females with acne, due to triggering factors such as hormonal imbalance, stress, and diet.
There are many reasons adult females can get acne. Hormonal disturbances caused by pregnancy, menstrual cycle, menopause, and oral contraceptives can contribute to acne by modifying the production of certain hormones. These hormones stimulate oil production within the skin, promoting the growth of acne-causing bacteria. Stress can increase the production of substances that activate oil glands within the skin of acne patients. Consumption of dairy and high-glycemic foods is also linked to acne. Certain hair or skin products can clog pores and cause comedonal acne (blackheads and whiteheads). A board-certified dermatologist can help determine the appropriate treatment for the type of acne you have.
Consequences of adult acne and scarring
The extent to which acne causes emotional distress varies, and is not related to the severity of the acne or acne scars. Some women with acne may experience disruption in their personal and professional lives as they fear stigmatization in relationships and employment. Adult females may also be more likely to seek treatment for active acne when acne bumps and scarring persist.
Acne scarring can be disfiguring. Permanent changes in skin texture in the form of pits or raised scars may not be easily concealed with makeup. Raised scars may also lead to skin picking and worsening skin texture and pigment.
Acne can also heal with red or dark spots that may not resolve for weeks to months. The dark spots may persist even longer without proper sun protection, especially on darker skin. Having both acne and dark spots may negatively impact one’s quality of life and self-perception.
The emotional toll associated with acne may include an elevated risk of developing depression compared to patients who do not have acne. Clinical studies show that having severe acne can negatively affect quality of life on par with long-term diseases such as arthritis, diabetes, back pain, and asthma. If you have acne, extensive scarring, or dark spots of any severity that are affecting your mental health, you may benefit from earlier intervention with oral medications.
What are options for treatment and support?
Acne is a medical condition, but it only needs to be treated if the acne or marks left behind from it are bothersome to you. Please see a board-certified dermatologist (in person or virtually) for the best available options if you wish to seek treatment.
Your dermatologist may prescribe a combination of topical (skin) and oral treatments. Some of these medications may not be appropriate if you are pregnant or breastfeeding, or carry risks. Ask your dermatologist about hair and skin products that may be irritating, clogging pores, or promoting oil production in the skin, making your acne worse. Also, avoid skin picking to prevent scarring, and try to minimize emotional and physical stressors.
For individuals with dark spots or scarring, consult a board-certified dermatologist to get a personalized treatment geared to your skin concerns. Use a broad-spectrum, tinted sunscreen daily and reapply it every two hours to help prevent acne marks from worsening. If your acne is causing you significant mental distress, ask your doctor about mental health resources. Additionally, seeking treatment for your acne may help you feel better. Consider joining online or in-person support groups in your area.
For more information, visit the American Academy of Dermatology Acne Resource Center.
Follow Dr. Nathan on Twitter @NeeraNathanMD
Follow Dr. Patel on Twitter @PayalPatelMD
About the Authors

Neera Nathan, MD, MSHS, Contributor
Dr. Neera Nathan is a dermatologist and researcher at Massachusetts General Hospital and Lahey Hospital and Medical Center. Her clinical and research interests include dermatologic surgery, cosmetic dermatology, and laser medicine. She is part of the … See Full Bio View all posts by Neera Nathan, MD, MSHS 
Payal Patel, MD, Contributor
Dr. Payal Patel is a dermatology research fellow at Massachusetts General Hospital. Her clinical and research interests include autoimmune disease and procedural dermatology. She is part of the Cutaneous Biology Research Center, where she investigates medical … See Full Bio View all posts by Payal Patel, MD
